Advancements in Nanotechnology for Restorative Dentistry
Nanotechnology is rapidly emerging as one of the most favorable technologies, which is gaining tremendous impetus due to its capability in modulation matter at smaller and smaller level. The nanotechnology drastically changes the chemical, physical, and mechanical properties of materials, changing their application in different fields as per the requirement. Advancements in nanotechnology are paving the future of dentistry as the nanomaterials have the potential to improve health care of dental patients. The nanomaterials have unique and superior properties which makes them highly advanced and vital for rapid diagnosis and treatment of various dental problems. Nanotechnology is being widely integrated into restorative dentistry for preventing and managing caries. Research has established the safe use of nanomaterials on human, which is attributing to their growing adoption by dental professionals and increasing acceptance from patients.
The growing application of nanotechnology in restorative materials has increased the quality and life of dental restorations, which result in better oral care and hygiene for patients opting for the treatment. Nanotechnology utilizes nanoparticles that are synthesized either from plants or chemically.
Applications of Nanotechnology in Restorative Dentistry
Tissue Engineering
Nanoscale fibers are widely used in tissue engineering, which involves the placement of implants that are biologically and physiologically more stable than previously used implants. As the ceramic materials do not have sufficient mechanical endurance, the nanoparticles are used to enhance the mechanical properties of these materials. The range of dimension of nanoparticles is same as that of cellular and molecular components, which help provide better results to the patients.
Tooth Repair
The nanotechnology stimulates the natural bio mineralization process to create the hardest tissue in the human body. Organizing highly organized micro architectural units of nanorod-like calcium hydroxyapatite crystals parallel to each other, the dental enamel can be created. Besides, the durability and appearance of tooth can be improved by replacing upper enamel layers with sapphire, which is 20-100 times harder than natural enamel or ceramic veneers. The sapphire can be made more fracture resistant as a part of nano structure composite material with the use of embedded carbon nanotubes.
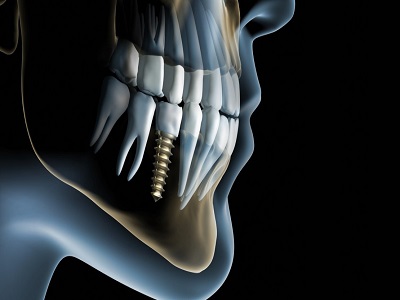
Dental Implants
Nanotechnology have rendered dental implant therapy as the most reliable option for the restoring the missing tooth. The natural bone surface has roughness of approximately 100 nm and roughing the implant surface at nanoscale level is essential for the cellular response that occurs in the tissue. The addition of nano-scale deposits of hydroxyapatite and calcium phosphate create a more complex implant surface for osteoblasts to develop. Thus, implants using nanotechnology can expedite bone growth and increase predictability and reduce time for osseointegration. Many in-vitro studies demonstrate that the nanostructured calcium coat increases the responsiveness of the bone around the implant. In addition, the nanoscale surface morphology augments the surface area, which provides more implant surface to react to the biologic environment.
Periodontal Drug Delivery
Triclosan-loaded nanoparticles developed by the emulsification-diffusion process is a novel delivery system for the treatment of periodontal diseases. Drugs can be incorporated into nanospheres composed of biodegradable polymer, which allows timed release of the drug as the nanospheres degrades, which allows for site-specific drug delivery. For instance, tetracycline is incorporated into microspheres for drug delivery in a periodontal pocket.
Dental Nanorobots
Dental nanorobots are designed to move through teeth and surrounding tissues using specific movement mechanisms. These nanorobots are remotely controlled and can be driven using innocuous low-intensity magnetic fields. The nanorobots are more efficient at maneuvering in hard-to-reach anatomies, enabling better contemporary disinfection methods by increasing the depth of penetration of drugs. The nanorobots are effective against the Enterococcus faecalis bacterium biofilms inside the human tooth, reaching at tissue depths of 2000 microns. The WHO priority bacteria have the ability to become antibiotic resistant, hence using nanorobots eliminates the need for antibiotics.
A colloidal suspension containing millions of active analgesic micron-size dental nanorobot ‘particles’ are provided to the patients’ gingivae, which then reach the pulp via the gingival sulcus, lamina propria and dentinal tubules. The analgesic dental robots are then commanded by the dentists to shut down sensitivity in any particular tooth that requires treatment. After oral procedures, the dentist orders the nanorobots to restore sensation and relinquish control of nerve traffic. This way, the patient feels more at ease and the dentist have greater selectivity, controllability. Besides, no side-effects are associated with analgesic robots unlike local anesthesia.
Nano-fiber coatings
Human gingival fibroblast cells have the potential to align, proliferate and secrete collagen in the direction of nanofibers, which could help in forming a tight fibrous collar. The coating will protect the underlying osseous attachment from bacterial attack or breakdowns.
Nanocomposites
Nanocomposites are spherical 40 nm silica particles that fill in the spaces between the large glass particles and achieve a high filler density. These composites are smaller than the wavelength of visible light (380-740 nm). The nanocomposite filler materials organize the microstructure of the composite at the atomic and molecular level. Improving the interface, the nanocomposites promote stability and equal distribution of stress between tooth and filler. Besides, the high filler content provides superior mechanical properties and smooth surface that prevent plaque accumulation and gum irritation.
3M Filtek Supreme Universal Restorative developed by Sumitra Mitra turned out to be a breakthrough in the dental tech, which has made life easier for patients as well as dentists. The easy-to-use, light-cured technology for fillings is an itsy-bitsy cluster of nanometer-sized particles that actually mimic a tooth’s natural enamel.
Way Ahead
Nanotechnology in restorative dentistry is transforming the average person’s perspective of the dentist, which is full of apprehensions and fear since nano dentistry involves minimally invasive procedures. The dentist-friendly procedure leveraging nanotechnology are helping create a more dentist-friendly atmosphere over time. Besides, nanotechnology in restorative dentistry allows an unprecedented level of precision, be it for diagnosing, treating, and preventing dental ailments. More such advancements in the nanotechnology can help to create better outcomes for patients, preserving and improving human health as a whole.
Rise in geriatric population and increasing incidences of dental problems are positively influencing the demand for restorative materials. Besides, industry players are developing environment-friendly nanofillers using “green chemistry”, which is anticipated to provide lucrative opportunities for the restorative materials in the coming years.
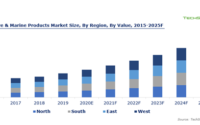
According to TechSci Research report “Restorative Dentistry Market – Global Industry Size, Share, Trends, Opportunity, and Forecast, 2017-2027 Segmented By Type (Posterior v/s Anterior), By Restoration Type (Direct v/s Indirect), By Product (Restorative Materials, Prosthetics, Implants, Restorative Equipment, Others), By End User (Dental Hospitals & Clinics, Dental Laboratories, Others), By Region”, the global restorative dentistry market is anticipated to grow at a formidable rate during the forecast period, 2023-2027. The market growth can be attributed to the rising awareness regarding dental hygiene and development of advanced technology such as Computer Aided Design and Manufacturing (CAD/CAM) software solutions. Besides, increase in personal disposable income of patients and increase in corporate dental practices are expected to boost the market growth in the coming years.